Knee arthroscopy procedure - Dr Jan Paradowski

I would like to invite you to our modern facilities in order to repair your knee with a completely professional, minimally invasional and safe procedure in a pleasant environment.
I conduct, among other procedures, complex arthroschopic procedures to sew the injured mensiscus. When that is not possible, or if you have already undergone a partial or total meniscectomy, we conduct an implant of the meniscus in its place (we prefer the most recent generation of synthetic meniscus ActiFit, injected during the operation with stem cells). It is also possible to transplanted an allograft of the meniscus (meniscus from a dead donor). We conduct the described arthroscopic procedure supplying the meniscus in keeping with the current guidelines presented at the 11th Worldwide Congress of the International Cartilage Regeneration & Joint Preservation Society (ICRS) by Prof. Peter Verdonk from Belgium – a world-renowned specialist in this area. This allows for the significant limitation of pain and a high risk of joint arthrosis after removal of the meniscus as well as the return of stability and function to the knee.
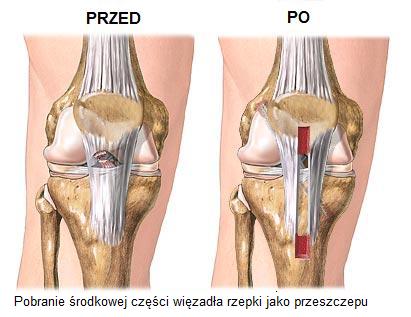
We also conduct arthoscopic procedures involving the reconstruction of the anterior cruciate ligament ACL (with the use of one’s own tendon – the classic method – or with the help of artificial ligaments Neoligaments Jewel ACL, which allows for the fastest return to sports activity). We also offer the full spectrum of arthroscopic joint cartilage reconstruction, using the new, most effective method: the Hyalofast hyaluronic pad in combination with Platelets Rich Plasma PRP GPS growth factors, Chondrocite (one’s own cartilage) that has been reproduced in the laboratory and injected into the damaged area of cartilage, reconstruction with the use of stem cells and scaffolds (synthetic scaffolding for the regenerating cartilage, e.g. MaioRegen - Dr. Elizaveta Kon, Bologna – dedicated to professional athletes with deep cartilage-bone injuries). We complete the operational procedure with regenerative/anti-inflammatory therapy appropriate for your case (Mesenchymal Stem Cells MSC, Orthokine therapy, platelet rich plasma PRP GPS growth factor injections). We make use of the latest discoveries in regenerative and reconstructive medicine. We are among the most experienced specialists in Poland.
ACL Reconstruction - click here
If you want to find out more about me, click here
If you want to sign up for a doctor’s appointment, click here
Read the following in this article:
- Advanced arthroscopy of the knee joint with reconstructive techniques
- Arthroscopy of the knee joint
- Indications for knee arthroscopy
- Preparation for operation
- Anaesthetic for the knee arthoscopy operation
- Knee arthroscopy: course of operation
- Post-operative steps
- Return to activity
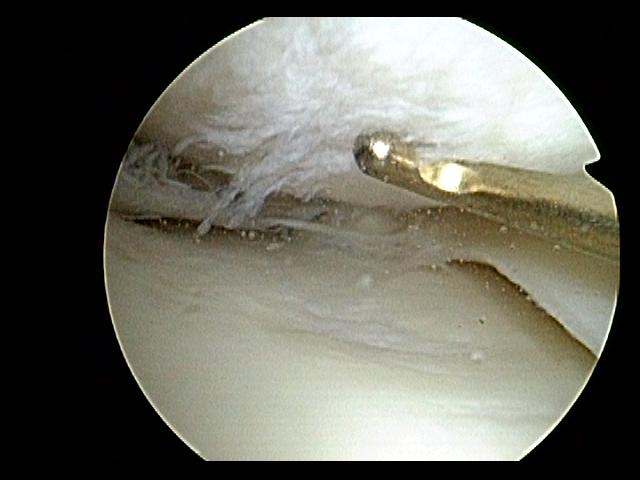
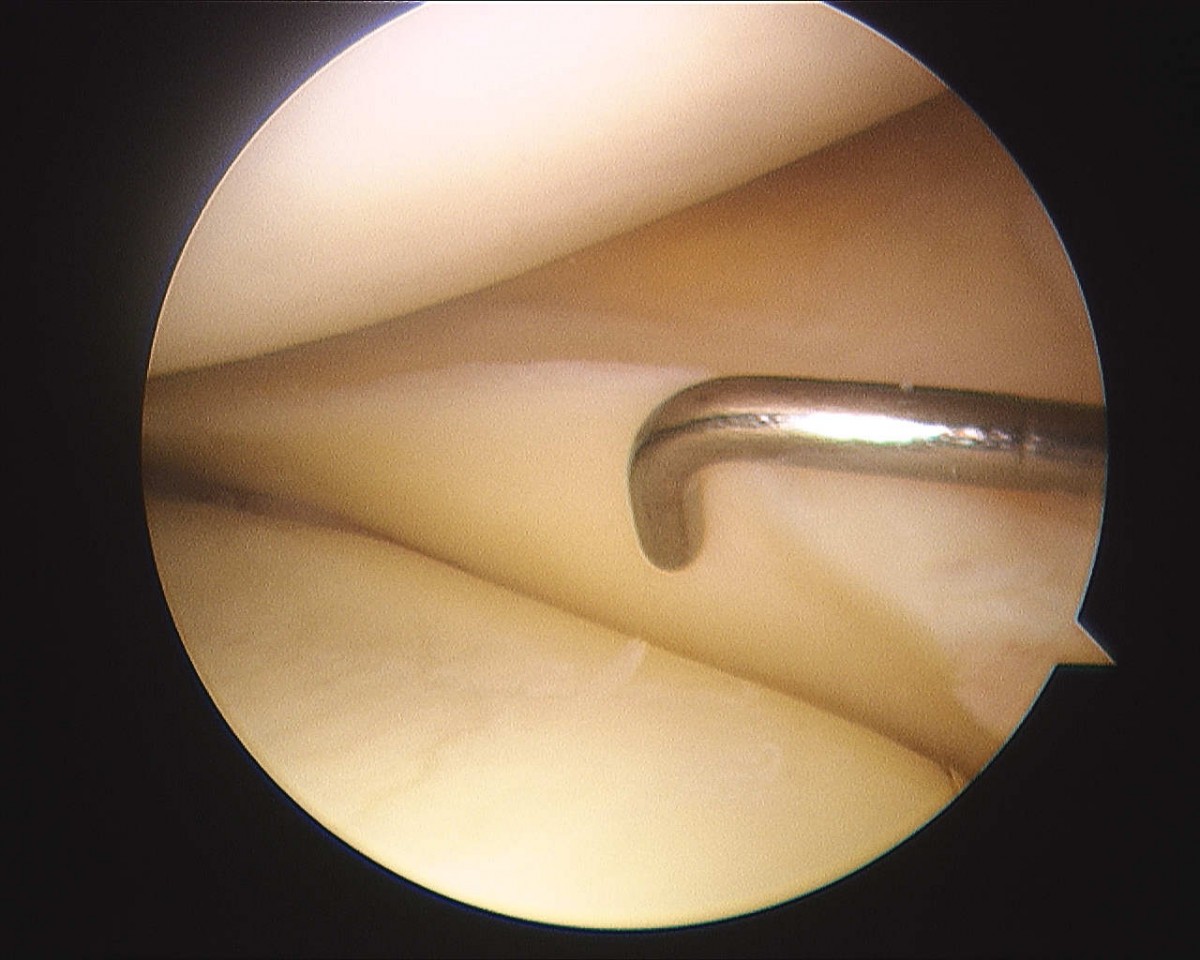
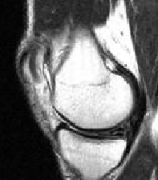 Each of our patients undergoes a detailed clinical-orthopedic exam before the arthroscopy procedure including other exams.
Each of our patients undergoes a detailed clinical-orthopedic exam before the arthroscopy procedure including other exams.
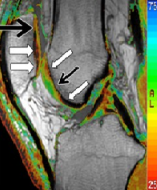
A huge role is played by the dynamic Ultrasound exam (conducted on the highest grade of instrument, in the real time of joint movement) and Doppler-Ultrasound (illustrates the increased flow of blood through the damaged area or inflamed tissue). We also obtain much essential information from magnetic resonance (MRI).
Read more about the exam and see how the knee ultrasound is conducted by Dr. Jan Paradowski. The specialized exam guidelines and modern resonance functions we utilize (e.g., t2-mapping using the highest detail for viewing tissue) allow for a precise, individually-planned operational procedure.
 Dr Jan Paradowski will go over with you in detail the entire process of diagnosis and will propose appropriate treatment. During the visit you will also have time to ask any questions important to you.
Dr Jan Paradowski will go over with you in detail the entire process of diagnosis and will propose appropriate treatment. During the visit you will also have time to ask any questions important to you.
Advanced arthroscopy of the knee joint with reconstructive techniques
Arthroscopy is a minimally-invasional procedure, which means greater comfort for the patient, speedier return to ability and minimal operational risk. Two small cuts in the skin on the sides of the kneecap are approx. 4-5 mm in length and often remain almost invisible after healing. During the qualifying doctor’s visit the patient is always informed in detail regarding the type of operation and its course. Additionally, simple preoperational preparation guidelines are transmitted. The arthroscopy itself is short (about 30 minutes), although it depends on the procedure. For example, a cartilage reconstruction procedure may last about 1 hour. The patient is sent home on the day of or the day after the procedure. Stitches are removed after about 8 days – this is a completely painless procedure.:
- medial and lateral mensicus (MM and ML)
- joint cartilage (using the latest operational techniques and successes of regenerative medicine)
- anterior and posterior cruciate ligament (ACL and PCL)
- removal of free bodies (osteochondritis dissecans, fragments of damaged meniscus, torn fragment of the joint cartilage through injury)
- removal of synovium (in conditions of the overgrowth of the synovium, e.g., in rheumatoidal illnesses or overgrowth of the synovium folds, e.g., in changes due to overload)
- in professional athletes,
- and in arthrosis (the accepted method of treatment of pain connected with knee joint arthrosis - debridement, or the removal of tissue fragments floating over the joint, shaving of overgrowth due to inflamed tissue, removal of osteophytes, often allowing for increased joint mobility, joint washing- removal of inflammatory agents floating internal to the joint).
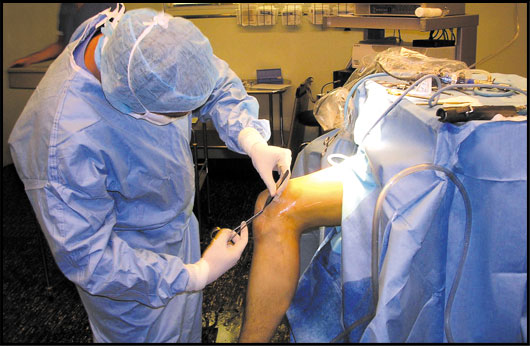
Arthroscopy of the knee joint
 Arthroscopic surgery has evolved over the last fewedecades, becoming an integral part of orthopedics. Knee arthroscopy is decidedly the least invasional, and is characterized by a high effectiveness in treatment and return to full ability.
Arthroscopic surgery has evolved over the last fewedecades, becoming an integral part of orthopedics. Knee arthroscopy is decidedly the least invasional, and is characterized by a high effectiveness in treatment and return to full ability.
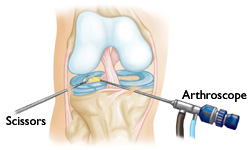
What in fact is arthroscopy itself? The name is derived from two Latin words – „Arthros” – joint, and “scope” – to view. Therefore, this means viewing the interior of the joint with the use of an endoscope. The procedure involves inserting the arthroscope (a form of endoscope – that is, a small tube containing a lens and fiber optic camera) through a small cut maximally 4mm in size into the knee. A special camera located in the arthroscope sends the picture from the examined joint, thus the interior of the joint is visible on the television monitor. The procedure allows for an exact viewing of the knee joint from the inside and performance of the required medical procedures. (This method is perfect for diagnosing and treating knee joint arthrosis.) The size of the arthroscope is individually chosen based on the joint examined. In the case of the knee joint this is usually a tool approx. 4-5 mm in width; that is why the incision is minimal.
This medical procedure causes less tissue damage, is less painful and guarantees quicker return to activity.
Indications for knee arthroscopy
Arthroscopy may be helpful in the diagnosis and treatment of many orthopedic conditions. We may be dealing with operational arthroscopy or diagnostic arthroscopy conducted in order to identify the condition.
Indications to conduct a procedured
- Damage to the knee joint ligament (torn meniscus) – the goal of the operation may be to treat the meniscus, when possible, or to remove damaged elements.
- torn and damaged anterior or posterior cruciate ligament (ACL and PCL)
- inflammation or damage to the synovium (the lining around the joint)
- dislocation of the kneecap
- removal of segments of broken cartilage in the knee joint
- removal of Baker’s cyst – fluid-filled cyst in the bursa under the knee. This situation often arises when there is pain and swelling, which can occur for other reasons, such as arthritis
Preparation for operation
Two weeks before the procedure:
The doctor conducts an interview with the patient in order to determine whether the given patient qualifies for operation (if there are problems such as heart failure, emphysema, diabetes or high blood pressure, they should be minimalized in order to conduct the procedurę. The preoperational assessment of patient’s health includes a physical exam and blood and urine exam. For patients who have had problems with their heart or lungs and for individuals over 50 years of age, conducting an ECG or X-ray of the chest is recommended.
The doctor may decide the discontinuation of certain medications that obstruct blood clotting, including: aspirin, ibuprofen, naproxen or other drugs.
The doctor will advise what medicines should be taken on the day of the procedure; that is why it is essential to indicate the medicines to which we have an allergic response.
It is necessary to inform the doctor about the amount of alcohol consumed, particularly if this was a large amount, particularly during the two weeks before the procedure.
For smokers, reducing or stopping smoking is recommended, because nicotine can cause wounds to heal more slowly
It is always necessary to inform the doctor about all inflammation points in the body.
On the day of the procedure:
- It is recommended to refrain from drinking or eating 6-12 hours before the procedure.
- After consultation with the doctor, the agreed-upon medicines may be taken.
Anaesthetic for the knee arthroscopy operation
The type of anaesthetic is chosen individually for each patient, depending on their state of health and the planned procedurę. In the case of arthroscopy of the knee the following anaesthetics are usually used:
- subarachnoid/epidural anaesthesia – is located in the lumbar area of the spine. The patient is conscious during the procedure in the case of this type of anaesthetic.
- general anaesthetic – the patient is not conscious during the operation.
Knee arthroscopy: course of operation
After appropriate anaesthetic the procedurę may begin. A proper incision is made through which the arthroscope is inserted, and the knee is filled with fluid (physiological saline). The surgeon may observe the knee joint continuously on the monitor screen with the help of a camera located in the arthroscope. During the procedure, if necessary, additional surgical instruments are introduced through the arthroscope located in the knee joint. These instruments may be used for cutting, removing or sewing the damaged tissue. After finishing the procedure the arthroscope is removed, the physiological saline solution removed, and the incision is closed and protected with a sterile bandage.
The risk in the case of knee joint arthroscopy is minimal. In the case of anaesthetic, side effects may be: an allergic reaction to the medicine or problems with breathing. As in the case of every operation, there is risk related to bleeding and infection. Additional postoperative complications include, among others, bleeding in the knee joint, blood clot in the leg, damaged cartilage, meniscus and ligaments in the knee, damage to the blood vessels or nerves, infection or stiffness in the knee.
Postoperative steps
Arthroscopy does not require hospitalization; that is why the patient may return home as soon as several hours after the procedurę. The knee joint that underwent surgery will be properly protected with a bandage. After the procedure the patient should take medicine according to the doctor’s recommendations.
Return to activity
The majority of patients are able to return to performing normal activities several weeks after the procedurę, without experiencing effects of the procedure.
Swelling of the knee is possible from 7-15 days after arthroscopy. This is completely normal and is no reason to fear! What is crucial is to maximally relieve the knee until the time of swelling absorption. The postprocedure knee may bear weight only after one week after the procedure. Patients may perform most daily activities without pain and fear of putting weight on the knee as early as the first month after the procedure. Depending on the level of complexity of the procedure the doctor will advise how to prepare the operated knee for normal function. Complete return to health may last from one month to a year, depending on the type of procedure, age, and rehabilitation undertaken. It is recommended to use orthopedic crutches for 6-8 weeks after the procedure.
In order to qualify for a knee arthroscopy and prepare a rehabilitation plan, I invite you to make an appointment for a doctor’s visit here
I perform all procedures in the comfortable environment of the Cracow clinic. My patients always remain under the personal care of qualified rehabilitation specialists.




