Contents:
- Major reasons for hip joint alloplasty
- Types of hip joint endoprostheses
- Endoprosthesoplasty: course of procedure
- Benefits of hip joint endoprosthesis
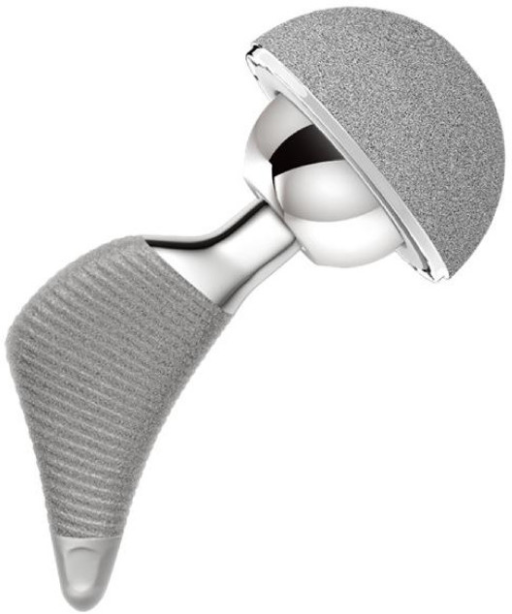 The most important indication to perform an endoprosthesoplasty of the hip joint is the elimination of pain and return of proper functioning to the arthritic joint. A successful endoprosthesis procedure offers the patient the opportunity to return to activity and painlessly perform all daily tasks. It is not without reason that endoprosthesoplasty is considered one of the greatest achievements of medicine in the prior century, as it is a chance for the patient to return to full activity. Worth remembering, however, is the fact that this is a significant operation, with a massive cutting of bone and the risk of complications (loosening of the endoprosthesis, infection and clotting complications – which can even be fatal). That is why SPORT-MED Center for Regenerative Medicine offers less invasive implantation of cutting-edge endoprostheses with minimal incision in the bone tissue.
The most important indication to perform an endoprosthesoplasty of the hip joint is the elimination of pain and return of proper functioning to the arthritic joint. A successful endoprosthesis procedure offers the patient the opportunity to return to activity and painlessly perform all daily tasks. It is not without reason that endoprosthesoplasty is considered one of the greatest achievements of medicine in the prior century, as it is a chance for the patient to return to full activity. Worth remembering, however, is the fact that this is a significant operation, with a massive cutting of bone and the risk of complications (loosening of the endoprosthesis, infection and clotting complications – which can even be fatal). That is why SPORT-MED Center for Regenerative Medicine offers less invasive implantation of cutting-edge endoprostheses with minimal incision in the bone tissue.
Dr. Jan Paradowski also uses Stem Cell Therapy to treat hip pain. We are the only medical center in Poland to use a combination of modern therapies, which together with the use of Mesenchymal Stem Cells (MSC) often allow patients to avoid the operation process completely or extend the period of functioning of their own joint. If necessary, we also have the ability to conduct a similarly less invasional hip arthroscopy treatment (endoscopic treatment), and we augment that with Stem Cell Therapy. We improve the range of movement, remove pain and return the patient’s ability to perform daily activities. If you would like to find out more and take advantage of the capabilities of modern medicine, contact us by clicking here.
Have a look at our facilities - click here.
Major reasons for hip joint alloplasty
Diseases that most often lead to the damage of the hip joint, and in consequence to the implantation of an artificial hip joint (endoprosthesoplasty) are:
► Age-related and/or strain-related degenerative arthritis
One of the most common hip joint problems is degenerative arthritis. Degenerative arthritis of the hip joint is the second most common arthritic problem (after the knee joint), resulting from the degeneration of joint tissue due to many factors. After many years of cumulative wear and tear, the joint tissue loses its ability to buffer and reduce friction, the result of aging and years of pressure on the joint. For myself as a sports doctor, professional athletes are an interesting case, because unfortunately, after many years in their career they meet up with arthrosis, and consequentially require individually-chosen specialized treatment (injections, ultrasound-guided intervention, Orthokine therapy, rehabilitation programs) – until we make a joint decision regarding an operation.
Initial symptoms of the disease may be subtle, but they decidedly signal a developing problem in the joint. Patients in the early stages of degenerative arthritis of the hip joint often complain of minor pain, weakening of the limb, reduced effectiveness in walking, as well as related pain in the knee joint. With progress of the disease, however, the symptoms become aggravated. Degenerative arthritis of the joints causes pain, swelling and reduces the movement in the joints; and as a result in the last stage of the disease patients are almost completely unable to move and perform daily activities.
Read more about degenerative arthritis of the hip joint - click here.
► Rheumatism
The hip joint is also very often damaged as a result of rheumatoid arthritis. Chronic inflammation leads to changes around the synovium, causing it to swell initially and then irreversibly enlarge. Changed synovial fluid damages the joints largely via two mechanisms: reduced anti-frictional characteristics (despite a pathologically increased amount of liquid) as well as inflammatory factors in the fluid that damage the tissue. The developing inflammation leads to significant, irreversible deformation of the joint, limitation of its movement, disappearance of joint tissue (erosion, softening – chondromalacia, nodal cavities) increased pain and cramping of the tendons and muscles, resulting in progressive physical disability. Summing up, the basic symptoms of rheumatic arthritis are:
- joint pain
- pain in the joints while moving and
- reduced range of movement.
It often happens that the joints develop increased fluid (produced by the inflamed synovial membrane) and are deformed (ostephytes – bone growths, bending of the extremity axis).
The joint cartilage tissue is damaged as a result of this inflammation, and may require the performance of hip joint allopasty (endoprosthesoplasty).
►Bone fracture in the hip joint area
One of the most common hip fractures is the femoral neck fracture, which takes place in the area where the hip bone enters the hip joint. Most often the elderly suffer from a femoral neck fracture, which may be one of the complications of osteoporosis (the disease characterized by reduced bone mass, reduced mechanical resistance and increased susceptibility to breaking caused by aging). Despite the fact that a significant majority of breaks in the hip bone occur among the elderly, they may also occur in younger people as a result of a serious injury. Hip joint alloplasty (the implant of an endoprosthesis) is a way to treat this type of break. In younger people, the fractured bone may sometimes be rejoined using screws.
►Genetic factors precluding other changes
Anatomical disorders lead to improper joint biomechanics and resultant destruction of the joint cartilage and early development of degenerative arthritis of the joint. This takes place in dysplasia of the hip joint, for example.
Types of hip joint endoprostheses
Alloplasty (endoprosthesoplasty) or endoprosthesis implant operation is a procedure that replaces the damaged hip joint with an artificial joint or endoprosthesis. Hip joint endoprostheses in current use may be divided into three types, cemented, cementless, and hybrid, depending on the form of junction with the bone substrate. I make the decision regarding the use of a given type of endoprosthesis during an individual orthopedic qualifying examination of the patient. Input into the qualification decision is derived from a medical exam, X-ray exam results, and sometimes computer tomography, magnetic resonance (MRI) and scintigraphy. I choose the endoprosthesis individually for each patient.
We distinguish the following types of endoprosthesis:
Cemented endoprosthesis – this type of prosthesis is cemented to the bone with the use of bone cement, a special bone “glue.” The cemented endoprosthesis is usually used in elderly patients with osteoporosis and rheumatoid arthritis.
Cementless endoprosthesis – this prosthesis is implanted into the bone, so that after the operation it grows into the bone over time. It is designed for younger patients whose bone foundation is good enough.
Each of the endoprostheses used in alloplasty are made of two parts, replacing the femoral head and neck: one part is set in the pelvis (the socket of the damaged hip joint) and the second in the hip.
Because of the increasingly younger age of people seeking the highest level of activity and quality of life and demanding endoprosthesoplasty of the hip joint, capoplasty has been very popular. This hip joint endoprosthesoplasty procedure recreates the hip joint surfaces. It is characterized by low bone loss during implantation and allows for the future replacement of the cap with a classic endoprosthesis after its attrition. Many orthopedists assume, however, that the patient should be offered a modern short-stem prosthesis. After it grows into the bone, it permits high physical activity with relatively low bone loss, because the element implanted into the degenerated femur replacing the femoral head and neck is short.
Endoprosthesoplasty: course of procedure

Implantation of the hip joint endoprosthesis
The endoprosthesis implantation procedure is performed with an epidural anaesthetic; general anaesthesia is rarely used. Before the procedure the patient receives an antibiotic for protection and low molecular weight heparin, minimalizing the risk of thrombosis. After the procedure, it is sometimes necessary to administer up to two units of red blood cells due to the loss of blood during the procedure and the post-operative period. It is also possible to conduct an auto transfusion of the patient’s own blood, which is taken two weeks before the operation.
At the start of the operation, the femoral neck and head are surgically removed. Then, the socket of the pelvic bones is deepened. The elements removed from the patient’s joint are replaced by the two-part endoprosthesis – the hip and socket elements. The articulations (new artificial joint surfaces) are formed by the head (ceramic or metal, placed on the hip element) and a polyethylene liner of the socket.
Antibiotic protection is used for 3-4 days after the operation, while anticoagulation protection is used for six weeks after the operation. As soon as the following day after the operation, the patient performs isometric and breathing exercises and makes attempts to stand up. These exercises are enhanced in stages so that on the 6 or 7 day, the patient is able to begin walking with limited weight placed on the operated limb. The patient remains in hospital after the operation for 1-2 weeks. This time is necessary for postoperative wounds to be healed and the rehabilitation process to be conducted. After leaving the hospital, the patient should walk using orthopedic crutches and continue exercising under the eye of a rehabilitation specialist, or in keeping with a specialist’s recommendations at home.
Rehabilitation is an extremely crucial element in returning to full activity – after the operation, the patient should perform systematic rehabilitation for a minimum of 6 weeks.
Possible post-operative complications
In spite of the fact that endoprosthesoplasty is a fundamentally safe procedure, as with any operation, complications may occur. The majority of complications, however, may be avoided with appropriate medical treatment and rehabilitation.
The most common complications are:
- Thrombosis (caused by lack of movement in the period of time around the operation)
- Infection (of the skin and tissues near the prosthesis)
- Sprains and fractures
- Loosening of the prosthesis
- Change of leg length
- Stiffening of the joint
Benefits of hip joint endoprosthesis
Foremost, the hip joint endoprosthesis allows patients to completely free themselves from pain and use of painkillers. The return of postoperative patients to physical activity depends on their age, condition, and the intensity of rehabilitation. What is most important, after the hip endoprosthesis implant, patients regain movement in the hip joint, and after proper rehabilitation, it is possible to practice sports.
Endoprosthesoplasty continues to be a dynamically developing area in orthopedics. Artificial joint elements are continually improved, and are more anatomical and resilient. Thanks to this procedure, the hip joint endoprosthesoplasty procedure is successful in more than 90% of patients!
Hospital stay
During the patient’s first day in the hospital, all necessary pre-operative tests are conducted. Patients can count on comfortable conditions and a high standard of medical care, which guarantees both use of the latest techniques, materials and equipment. Highly-qualified doctors, physiotherapists and medical staff offer the best level of care. In addition to medical tests the patient will be examined by an orthopedist, internist and an anesthesiologist, who will choose the appropriate type of anaesthetic. As soon as the first day after the operation, the patient begins their custom-designed rehabilitation, which they learn to perform so that they can do it at home during the rehabilitation period after leaving our clinic.
Cost
The complete cost of the endoprosthesoplasty procedure includes the cost of the prosthesis, hospital stay, doctor and medical staff care as well as the cost of the operation, which makes used of the best materials. The cost is set after becoming familiar with the patient’s disease history and is individually established for each patient.
In order to qualify for a hip joint endoprosthesoplasty procedure and prepare a rehabilitation plan, I invite you to make an appointment for a doctor’s visit with me by clicking here.




